
Review of Ophthalmic Managed Clinical Networks (MCNs) in Staffordshire and Shropshire
The aim of the MCNs is to bring together primary care optometrists with local ophthalmologists within a geographical area. This is a review Strategy Unit were commissioned by NHS England to work with a medical retina MCN in Shropshire, Telford and Wrekin and a glaucoma MCN in Staffordshire and Stoke on Trent, to review their work so far and look at the opportunities the networks present.

Evaluating and embedding social values in procurement at East London NHS Foundation Trust
This report presents emerging findings from the early development stages of a social value approach to procurement by East London NHS Foundation Trust (ELFT). These findings provide insights for other organisations beginning to explore how to use procurement to contribute to improving health and reducing health inequalities.

Advancing the analytical capability of the NHS and its ICS partners
The Strategy Unit were asked by the Strategy and Development Team in the Directorate of the Chief Data and Analytics Officer, NHSE/I, to make recommendations for advancing analytical capability across the health and care workforce.

Estimating the impact of the proposed reforms to the Mental Health Act on the workload of psychiatrists
In January 2021, the Government published a White Paper, setting out its plans to reform the Mental Health Act.
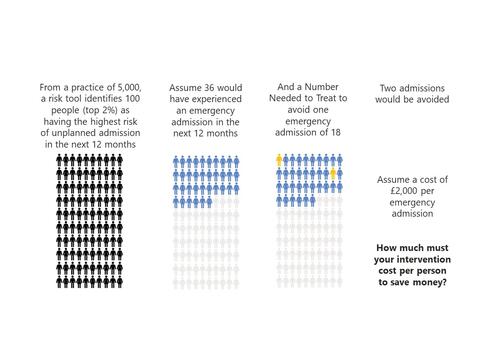
‘To risk stratify or not risk stratify, that is the question’ (At least, it should be)
Risk stratification tools are ubiquitous in healthcare. The concept is simple and seductive.

Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.
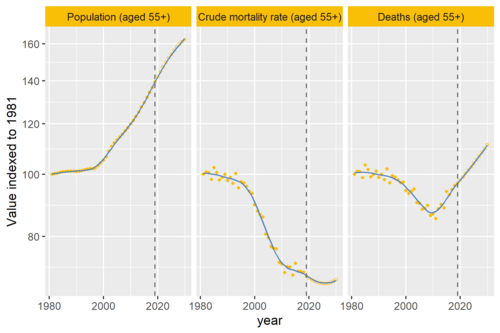
Why are deaths set to rise?
In our recent analysis of healthcare use in the last 2 years of life, we point out an important change that’s taking place to life and death in the UK.
Modelling the impact of covid on waiting lists for planned care
Working with the national collaboration to coordinate covid-related analysis, and the NHSE/I Midlands region, the Strategy Unit has produced a ‘systems dynamics’ model of waiting lists for planned care. The model is freely available for non-commercial use across the NHS. Here, Steven Wyatt and Mike Woodall explain what we did and how we did it.
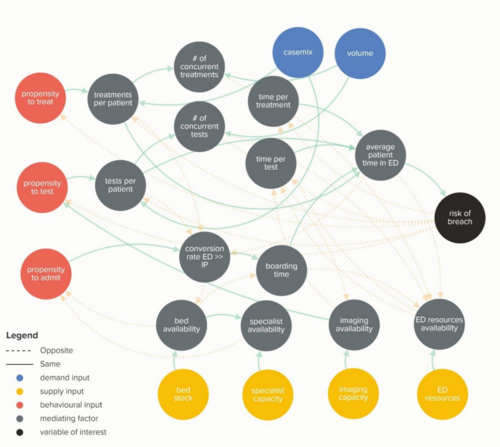
Waiting Times and Attendance Durations at English A&E Departments
In March 2019, NHS England is expected to report the outcome of its review of constitutional waiting times targets. This report reviews the factors that have led to the decline in performance against one of these targets - the 4-hour target for Accident and Emergency Departments. The analysis uncovers new insights and has the potential to reshape received wisdom about the performance of A&E departments, carrying important implications for healthcare policy and system leadership.
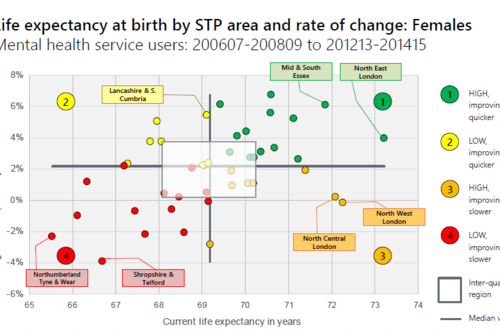
Making the case for integrating physical and mental health services in England - National overview
This is a national overview report of our Making the case for integrating physical and mental health services reporting which took place in July 20
Risk and Reward Sharing for NHS Integrated Care Systems
Risk and reward sharing is a simple and attractive concept, offering a commissioner the opportunity to co-opt and incentivise a provid
Scoping the Strategic Analytical Requirements for Clinical Neurosciences in England
Neurosciences encompasses a large number of services and interventions, delivered to individuals with a wide range of conditions by numerous provid
