
Want to ease pressure in urgent care? Simply cut community services!?!
What should decision makers do with analysis that challenges deeply held assumptions? In this blog, Fraser Battye reflects on a surprising recent finding about community services.

Ghosted by an old friend
“…personal contact was a vital element in general practice from the beginning. By 1959 50% of people in England regarded their GP as a personal friend.”

Learning about what works in urgent community response
The initial report from the national urgent community response (UCR) evaluation, along with an economic modelling tool to help service providers and systems understand the impact of UCR, is now available.

The NHS as an anchor institution: addressing fuel poverty
The number of households in fuel poverty in Staffordshire and Stoke-on-Trent (SSoT) is higher than the national average. As anchor institutions, NHS organisations can use their assets to influence the health and wellbeing of their local communities. The Strategy Unit was asked by the Midlands NHS Greening Board to evaluate a cross-sector initiative in SSoT to help alleviate fuel poverty using savings generated through solar panels on NHS buildings. The project is called Keep Warm, Keep Well.
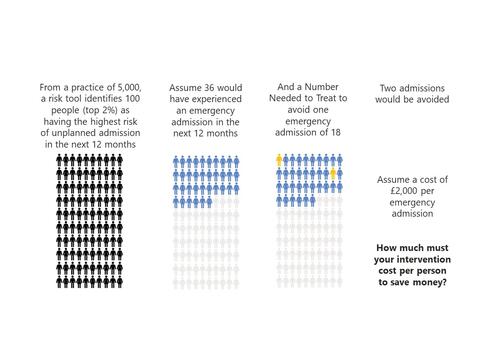
‘To risk stratify or not risk stratify, that is the question’ (At least, it should be)
Risk stratification tools are ubiquitous in healthcare. The concept is simple and seductive.

Infant feeding problems, lockdown and attendance at Emergency Departments: what’s going on?
From our previous work, with Nuffield Trust and Health Foundation, we know that lockdown had a significant effect on attendance at Emergency Departments (ED). We also know that this effect was very unevenly distributed: some demographic groups stayed away far more than others.

The impact of social care on demand for urgent hospital care: have we reached a consensus?
The care home COVID crisis and the effects of longstanding staffing and funding shortages has meant that social care has featured heavily in the media over the last 12 months.
Some positive news for integrating GP practices with hospital trusts
The drive for greater integration of health and care services has been the central theme of UK health policy for most of

Why community alternatives to hospital admission don’t (typically) reduce total admission levels
Repeatedly, published evaluations show that community/primary care services interventions with a stated intention to reduce total (or forecast total) emergency admissions to hospital don’t achieve the expected result**
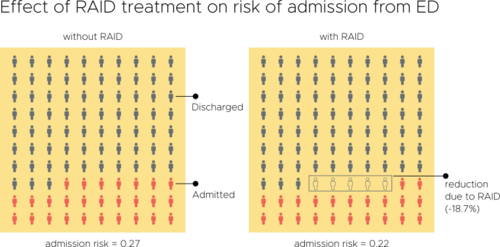
Evaluation of an Integrated Mental Health Liaison Service (Rapid Assessment Interface and Discharge Service) in Northern Ireland
A high proportion of patients treated for physical health conditions also have co-morbid mental health problems; and there is growing acceptance of
Horizontal or Vertical: Which way to integrate?
In 2011, Primary Care Trusts faced a difficult choice. The Transforming Community Services policy required a complete break of commissioner and provider functions. But what should PCTs do with the community health services they delivered; vertically integrate with an acute trust, horizontally integrate with a mental health trust, or set up a stand-alone community trust or Community Interest Company? Seven years on, this report explores the impact this choice had on the level and growth in emergency hospital use in older people and considers the wider implications for the NHS as it develops new models of care and integrated care systems

HSJ Article - Why are A&Es feeling the strain?
Article published by HSJ on 3rd November 2017.
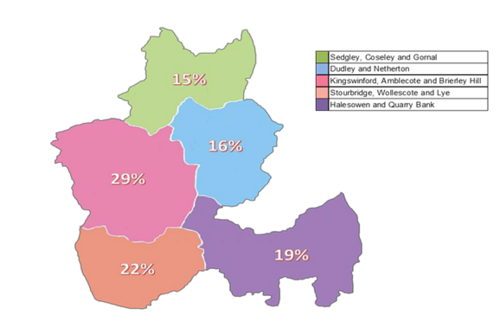
Evaluation of the Dudley Multidisciplinary Teams (MDTs) Summary of Final Report
Multi-disciplinary Teams (MDTs) in primary care are a core component of Dudley's care model; they are also widely used elsewhere.
Integrated Impact Assessment for Major Hospital Reconfiguration
The Strategy Unit worked as a strategic partner of the NHS Future Fit Programme in Shropshire and Telford and Wrekin from its initiation and u