
A collaborative partnership with the Health Foundation
The Strategy Unit is collaborating with the Health Foundation to help address key health and social care issues by combining our expertise in data analysis.
Diagnosing harms?
All medicines are poisons. Everything that cures could kill if administered in the wrong doses, to the wrong people, at the wrong times, in the wrong ways.
How is growth in diagnostic testing affecting the hospital system?
Diagnostic services, such as medical imaging, endoscopy, and pathology, have grown substantially in recent years and at a faster rate than most other healthcare services. Increased diagnostic testing brings benefits to patients, but rapid growth of this service area within a complex, adaptive system such as the NHS is likely to have had unintended consequences. Midlands ICBs wanted to understand the impact of diagnostic growth on hospital services.

Bringing patient flow modelling into general practice
With general practice appointments hitting the highest numbers on record (34.8 million in England alone in November 2021), careful organisation and planning for patient appointments is increasingly important.

Strategy Unit devises a new method for classifying outpatient appointments
The number of outpatient attendances in England is now approaching 100 million each year.

Measuring the effect of the coronavirus pandemic on population health
Measuring the effect of the coronavirus pandemic on population health

Less noise and more light: using criteria-driven analysis to tackle inequalities
Reducing health inequality is a long-standing aim of health policy. Yet the gap between policy aim and population outcome has grown in recent years: on most measures health inequalities have got worse.
Socio-economic inequalities in access to planned hospital care: causes and consequences
Tacking inequalities in health is a long-standing NHS policy objective. Variation in the experiences and outcomes of different communities during the COVID-19 pandemic served to bring this issue back into focus.
Analytical Collaboration for COVID-19
Between March and December 2020 the Health Foundation; King’s Fund; Nuffield Trust; and the Strategy Unit collaborated to provide
Strategy Unit analysis of air quality highlights inequalities
Poor air quality is the largest environmental risk to public health in the UK and central London has the highest levels of particulate matter and nitrogen dioxide. The Guy’s and St. Thomas’ charity, now operating its programmes under the Impact on Urban Health banner, have committed to 10 years of funding to improve air quality-related health in the residents of South London boroughs of Lambeth and Southwark. The charity commissioned the Strategy Unit to explore the health of several key groups and the factors that most influence health alongside air quality within the area.
Strategy Unit releases opensource model for planning vaccine centre capacity
The UK is running its largest ever vaccination programme. The stakes are enormous.
Mental Health Surge Model
Early in the Covid pandemic, it became clear that people’s mental health would suffer. Whether through bereavement, unemployment, social isolation, not being able to access support services – or a host of other routes – an alarming picture began to emerge and attract attention.

Socio-economic and environmental impact of Herefordshire and Worcestershire STP
Anchor institutions are large, typically non-profit, public sector organisations whose long-term sustaina

Accessibility of perinatal mental health services for women from Ethnic Minority groups
Barriers to accessing mental health care during pregnancy and the first postnatal year (perinatal period) seem to be greater for ethnic minority women.
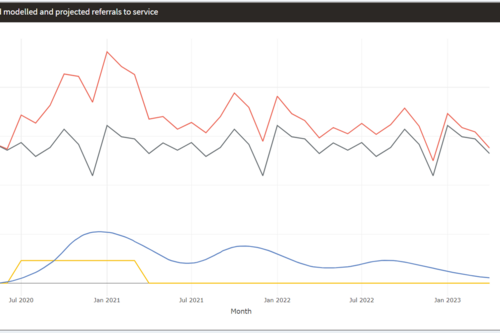
Modelling the impact of covid on waiting lists for planned care
Working with the national collaboration to coordinate covid-related analysis, and the NHSE/I Midlands region, the Strategy Unit has produced a ‘systems dynamics’ model of waiting lists for planned care. The model is freely available for non-commercial use across the NHS. Here, Steven Wyatt and Mike Woodall explain what we did and how we did it.
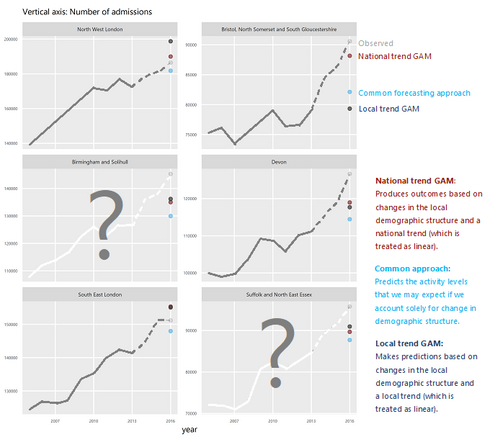
How will we know if Integrated Care Systems reduce demand for urgent care?
The implications of a blended payment system are far reaching: Decisions about planned activity levels will determine the total funding envelope for urgent care within a system and will influence the behaviour of healthcare providers and the services they deliver to patients.
Risk and Reward Sharing for NHS Integrated Care Systems
Risk and reward sharing is a simple and attractive concept, offering a commissioner the opportunity to co-opt and incentivise a provid
Identifying Potential QIPP Opportunities - Dudley Example
Given the pressures within the NHS, being able to identify opportunities for efficiencies and improvements is
Making the Case for Integrating Mental and Physical Health Care - Full Report.
An analysis of the physical health of people who use mental health services: life expectancy, acute service use and the potential for