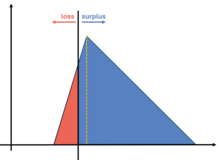
Contracting for health outcomes: from concept through theory to implementation
In this new report, jointly authored with colleagues from the University of York and The Royal Orthopaedic Hospital NHS Foundation Trust, we set out in detail how an outcomes-based contract for elective knee replacements might be constructed, and the potential implications for commissioners, providers, and policy-makers.

Playing our part in conversations about death
“Dad, why are all your ‘peptalks’ about death?” Children can be a source of fundamental insight. They seem to specialise in feedback of the unvarnished, unmediated and fully caffeinated variety. The kind of feedback that cuts straight to it. My youngest daughter, mid-way through our sunny walk down the hill to school, pressed on: “And you wear black all the time. You look like a crow…” Fundamental insight, and now fashion advice. This was quite the school run.

A Picture of End-of-Life Care in England
Working with Macmillan our analysis investigates who is more likely to experience poor outcomes associated with shortcomings in end-of-life care? Are there particular areas in England where those at end-of-life face significant challenges and how might the supply of services in an area be influencing these?

Diagnosing harms?
All medicines are poisons. Everything that cures could kill if administered in the wrong doses, to the wrong people, at the wrong times, in the wrong ways.

Inclusive Elective Care Recovery
These case studies present the key features and learning from local initiatives which championed inclusive approaches to elective care recovery.
How is growth in diagnostic testing affecting the hospital system?
Diagnostic services, such as medical imaging, endoscopy, and pathology, have grown substantially in recent years and at a faster rate than most other healthcare services. Increased diagnostic testing brings benefits to patients, but rapid growth of this service area within a complex, adaptive system such as the NHS is likely to have had unintended consequences. Midlands ICBs wanted to understand the impact of diagnostic growth on hospital services.
Socio-economic inequalities in coronary heart disease
There are substantial differences in mortality rates from cardiovascular disease between socio-economic groups. Our new tool provides an overview, for ICBs, of the points on the care pathway where inequalities emerge and are amplified

Helping ICSs to reduce inequalities in access to planned care
Are there inequalities in access to planned care? If so, what are they? Which groups ‘gain’ and which groups suffer? And what could be done to address any inequalities? In pursuing their objective of reducing inequalities, what could Integrated Care Systems (ICSs) do? What strategies and approaches are likely to be successful?

What matters when waiting? – involving the public in NHS waiting list prioritisation
As the NHS emerged out of the pandemic, it was confronted with the challenge of not only recovery of unprecedented waiting lists, but with inequalities which required attention. NHS leaders challenged providers to restore inclusively and at University Hospitals Coventry and Warwickshire NHS Trust, we have developed a way of doing just that, whilst simultaneously reducing waiting times for all.
Inequalities in access to healthcare - what’s our next move?
Our research, published in the Lancet Regional Health Europe, highlights substantial inequities in access to elective hip replacement surgery. We found no evidence that these inequities reduced between 2006 and 2016.
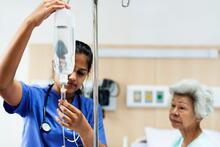
Strategies to reduce inequalities in access to planned hospital procedures
UPDATE 10th August: Now including briefing note for Integrated Care Boards on legal duties in respect of reducing inequalities. This report guides ICBs through the process.

Treating people on waiting lists: who decides what is fair?
Waiting lists for elective care are in the news. The national plan has been issued, with the expectation that lists will continue to rise for some years - and that long waiting will not disappear anytime soon. Addressing this ‘backlog’ will remain a fundamental challenge for some time to come.
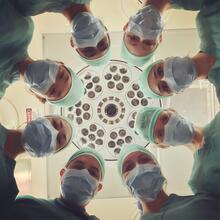
Decisions to admit patients are not solely determined by clinical risk
Whether or not to admit a patient is one of the most routine yet important decisions a doctor in an Emergency Department
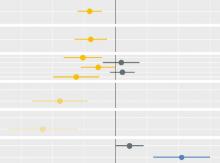
Socio-economic inequalities in access to planned hospital care: causes and consequences
Tacking inequalities in health is a long-standing NHS policy objective. Variation in the experiences and outcomes of different communities during the COVID-19 pandemic served to bring this issue back into focus.

Evidence review: Early diagnosis of cancer
Detecting cancers early is essential to saving lives and reducing the need for invasive treatments.
How can analysis help clinicians improve services? Interview with Dr Anna Lock
Dr Anna Lock, Justine Wiltshire and Lucy Hawkins reflect on the Strategy Unit's innovative end of life care analysis. How can this work help clinicians to improve services?

End of Life analysis: what next? A perspective from Catherine Walshe
‘In this world nothing can be said to be certain, except death and taxes’.

End of Life analysis: what next? A perspective from Seamus O'Mahony
In this blog, the author of ‘The Way We Die Now’ - Seamus O’Mahony – sets our findings into a broader context. He also examines one topic raised in our analysis: chemotherapy at the end of life.
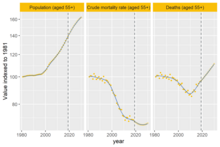
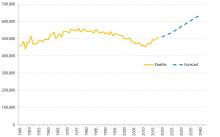
Why are deaths set to rise?
In our recent analysis of healthcare use in the last 2 years of life, we point out an important change that’s taking place to life and death in the UK.
Health service use in the last two years of life
Health and care services get just one opportunity to support people at the end of their life. When this support is compassionate and appropriate, unnecessary suffering can be avoided and grieving can be eased. When this is not the case, harm and distress can result. The difference in these experiences can be profound.